Precious Time
 Bella , 8, loves being her mother’s little helper. In November 2012, equipped with her own Bella-sized skimmer and brush, the two-year-old set out to clean her family’s backyard pool…by herself. And then everything that could go wrong, did go wrong.
Bella , 8, loves being her mother’s little helper. In November 2012, equipped with her own Bella-sized skimmer and brush, the two-year-old set out to clean her family’s backyard pool…by herself. And then everything that could go wrong, did go wrong.
Fortunately, everything started going right not long after her mother, Elysia, pulled an unconscious Bella from the water. Although Elysia’s cell phone had died, a neighbor’s father happened to pull up and called 911. An EMT in training was jogging by the house and took over CPR until help arrived. Then a ten-minute helicopter flight brought Bella to the emergency department at Baylor Scott & White McLane Children’s Medical Center where a team was waiting for her.
“I was in shock,” Elysia says. “I had no comprehension of the severity of it at that time. I just put my trust in those doctors, nurses and the first responders to just do what they needed to do.” Bella wasn’t breathing and had no heartbeat. Her body temperature was less than 88 degrees. “In that situation, time was of the essence. Luckily, someone suggested ECMO,” Elysia says.
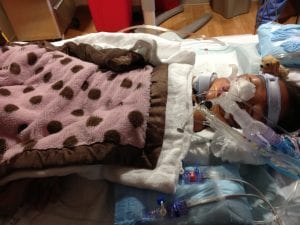 Extracorporeal Membrane Oxygenation therapy, or ECMO, isn’t generally the first tactic emergency physicians turn to. The ECMO machine takes over or partially supports the function of up to three organ systems: the heart, lungs, and kidneys. This allows those systems to rest and heal. “It is the most support you can be on,” says Joshua Greer, the ECMO program coordinator at McLane Children’s, “but you hope you don’t get to the point that you have to use it.”
Extracorporeal Membrane Oxygenation therapy, or ECMO, isn’t generally the first tactic emergency physicians turn to. The ECMO machine takes over or partially supports the function of up to three organ systems: the heart, lungs, and kidneys. This allows those systems to rest and heal. “It is the most support you can be on,” says Joshua Greer, the ECMO program coordinator at McLane Children’s, “but you hope you don’t get to the point that you have to use it.”
The McLane Children’s team brought the ECMO machine down to the emergency room for Bella, another diversion from the norm because of its size. The complicated machine can take up a whole room and didn’t fit in the elevator along with the gurney and staff, so Shelly May, RN, rode on top of the cart with the machine to monitor Bella.
“My hope was so grim,” Elysia says. “She’d gone without oxygen for so long that she would most likely never walk, never talk, and would need a feeding tube. But ECMO made the difference.”
ECMO took over for Bella’s lungs, oxygenating her blood as she breathed and allowing her lungs to rest. She was also kept in a medically induced coma to allow the swelling around her brain to heal. Luckily, the cool water of the pool helped preserve her brain function. “The problem has to be reversible,” Mr. Greer says. “ECMO doesn’t cure anything; it only buys time for healing.”
After three days, Bella recovered enough to discontinue ECMO therapy. “We see this quick recovery quite a bit. For instance, babies in the NICU might be on ECMO for days versus the ventilator for months,” Mr. Greer says.
 Bella stayed in the pediatric intensive care unit at McLane Children’s for just over two weeks before transferring to an in-patient rehabilitation program in Fort Worth for six months. “She had to relearn how to do everything from walking, talking, to feeding herself and chewing. It was almost like having an infant again,” Elysia says.
Bella stayed in the pediatric intensive care unit at McLane Children’s for just over two weeks before transferring to an in-patient rehabilitation program in Fort Worth for six months. “She had to relearn how to do everything from walking, talking, to feeding herself and chewing. It was almost like having an infant again,” Elysia says.
Now, at age six, Bella runs, rides a bike, speaks English and Spanish, and has no fear of water, according to her mother. “After a near-drowning, some children can walk and talk relatively normally, but most don’t even get that far,” Elysia says. “On the scale of recovery, no one looks like Bella and it’s because she was on ECMO.”
Although this military family is now stationed out of state, Elysia still keeps in contact with the McLane Children’s emergency room staff members who treated Bella. They also visit whenever the family is home, just so the staff can see Bella’s astounding recovery. “The emergency room staff doesn’t often get to see how they impact their patients in the long term,” Elysia says. “It’s important for them to know they do make a difference.”




